Navigating the journey of dental surgery can be daunting, especially when it involves complex procedures like dental bone grafts. Whether you’re getting ready for dental implants or need to correct bone loss due to periodontal disease, understanding the dental bone graft healing stages is crucial. This knowledge alleviates anxiety and equips you to take proactive steps in your healing process. In this blog, we will delve into what a dental bone graft for dental implant is, the preparation required for the procedure, and most importantly, the various stages of healing you can expect. Armed with this information, you’ll be better prepared to manage your recovery and ensure the long-term success of your dental graft.
Healing Stages for a Successful Graft
Understanding the dental bone graft healing stages can significantly impact the procedure’s short-term recovery and long-term success. It helps in mental preparation, optimising care, and facilitating effective communication with healthcare providers, all of which contribute to better outcomes.
What is a Dental Bone Graft?
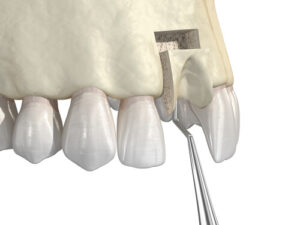
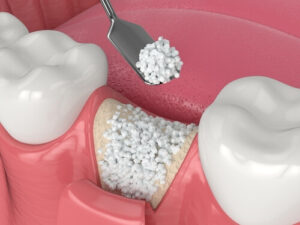
Dental bone grafting is a surgical procedure that involves transplanting bone tissue to an area of the jaw where bone mass has been lost. The graft serves as a platform for bone growth, allowing for more stable placement of dental implants or other restorative devices. It may also be essential for reconstructing areas that have suffered bone loss due to injury, infection, or long-standing dental issues like periodontal disease.
Why Is It Often Necessary?
Support for Dental Implants: One of the most common reasons for dental bone grafts is the need for a solid foundation for dental implants. Insufficient bone mass can make it difficult to place implants, risking implant failure securely.
- Periodontal Disease: Advanced gum disease can lead to bone loss in the jaw. A bone graft can help regenerate lost bone and provide better support for your teeth, improving aesthetics and function.
- Tooth Extractions: Sometimes, bone grafts are necessary after tooth extractions, particularly if you plan to replace the extracted tooth with an implant. The graft can help maintain the shape and volume of the tooth socket.
- Jaw Injury or Surgery: Accidents that result in jaw injuries may necessitate bone grafts to restore function and structure. Similarly, surgery to remove tumours or cysts often involves bone removal, and grafts can assist in rebuilding the affected area.
- Aesthetic and Functional Concerns: Bone loss in the jaw can affect facial structure, leading to a “sunken” appearance. A bone graft can restore a more youthful contour. Moreover, it can improve bite function and general oral health.
Different types of dental bone grafts
Dental bone grafts come in various types, each with its own set of advantages and limitations. The type of graft used often depends on the bone graft material, the specifics of your condition, the extent of bone loss, and the subsequent treatment plan. Here are the most common types of dental bone grafts:
Autografts (Autogenous Bone Grafts)
- Source: Your bone, typically from another part of your jaw, hip, or tibia.
- Advantages: The risk of rejection or allergic reaction is minimal since the healthy bone tissue is harvested from your body.
- Limitations: Requires two surgical sites, which may lead to a longer healing time and additional discomfort.
Allografts (Allogenic Bone Grafts)
- Source: Cadaver bone that has been treated and sterilised to ensure its safety.
- Advantages: Eliminates the need for a second surgical site, usually readily available.
- Limitations: Slightly higher risk of infection or rejection compared to autografts.
Xenografts (Xenogenic Bone Grafts)
- Source: Animal bone, usually bovine, that has been processed to make it compatible with human tissue.
- Advantages: Like allografts, xenografts eliminate the need for a second surgical site.
- Limitations: Risk of infection or allergic reaction, although this is generally low due to rigorous processing.
Alloplasts (Synthetic Bone Grafts)
- Source: Synthetic materials like hydroxyapatite or other biocompatible substances.
- Advantages: Readily available and eliminates the need for a second surgical site.
- Limitations: Some types may not integrate as well as natural bone, leading to possible complications.
 Growth Factors and Bone Morphogenetic Proteins (BMP)
Growth Factors and Bone Morphogenetic Proteins (BMP)
- Source: Laboratory-produced proteins that can stimulate bone growth.
- Advantages: Can be used in conjunction with other types of grafts to accelerate healing and bone growth.
- Limitations: Expensive and may require special approval for use.
Your dental surgeon will typically decide on the most appropriate type of bone graft based on your medical history, the specific dental procedure you need, and other factors like the availability of graft materials. Knowing the different types of dental bone grafts can help you engage more effectively in your treatment plan and set realistic expectations for the procedure and the subsequent dental bone graft healing stages.
Preparing for the Procedure
Preparation for a dental bone graft procedure is essential in ensuring the best possible outcome. Proper preparation can minimise complications, speed up the healing process, and contribute to the long-term success of the graft. Here are some key considerations:
Consultation and Pre-Operative Assessment
- Your dental surgeon will likely schedule a detailed consultation to discuss the procedure, the type of graft used, and the expected dental bone graft healing stages.
- Imaging tests like X-rays or CT scans may be conducted to assess the condition of your jawbone and surrounding structures.
Medical History and Medications
- It’s crucial to provide a complete medical history, including ongoing medications and allergies. Some medications, like blood thinners, may need to be adjusted before surgery.
Antibiotics and Pre-Medication
- Your surgeon might prescribe antibiotics to be taken before the procedure to minimise the risk of infection.
Dietary Restrictions
- You may be asked to fast for a certain period before the surgery if general anesthesia will be used.
- Discuss with your surgeon about post-operative dietary restrictions and prepare soft or liquid foods for the initial healing stage.
Oral Hygiene
- A clean oral environment is vital for successful grafting. You may be advised to have a professional dental cleaning before the procedure.
- You’ll likely be instructed to rinse your mouth with an antiseptic mouthwash shortly before the surgery.
Scheduling and Logistics
- Make sure to clear your schedule for the day of the procedure and, ideally, for a few days afterwards for the initial recovery.
- Arrange for someone to drive you home if you are undergoing sedation or general anesthesia.
Financial and Insurance Planning
- Dental bone grafts can be expensive, so review your insurance coverage and discuss payment options with your dental office beforehand.
By adequately preparing for your bone grafting procedure, you’re laying the groundwork for a smoother procedure and more effective healing. It also allows you to have an informed discussion with your dental surgeon, allowing for a more personalised and successful treatment plan.
 Dental Bone Graft Healing Stages
Dental Bone Graft Healing Stages
Understanding the dental bone graft healing stages is crucial for optimal recovery and the long-term success of the graft. Each stage has its own set of characteristics, care requirements, and potential complications to watch for. Any surgical or invasive procedure carries risks. Before proceeding, you should seek a second opinion from an appropriately qualified health practitioner. Here is a breakdown of the typical healing stages:
Immediate Aftermath: First 24-48 Hours
- Characteristics: Expect some pain, swelling, and possibly minor bleeding.
- Care: Strict oral hygiene, avoid touching the surgical site, and possibly take prescribed antibiotics and pain medication. A soft diet is recommended.
- Watch for: Excessive bleeding, severe pain, or signs of infection.
Inflammation and Soft Tissue Healing: Days 3-7
- Characteristics: The swelling generally peaks and then starts to subside. The gum tissue starts to heal.
- Care: Continue with medications as prescribed. Maintain excellent oral hygiene but avoid direct brushing of the surgical site. Rinse with salt water or antiseptic solutions is recommended.
- Watch for: Persistent swelling or pain, foul smell, or discharge, which could indicate infection.
Early Bone Formation: Weeks 2-6
- Characteristics: Initial bone formation begins around the graft material. The site may appear less red and more like normal tissue.
- Care: Gradually reintroduce harder foods into your diet. Continue with excellent oral hygiene.
- Watch for: Any signs of graft failure, like increased pain or loose bone grafting material. Consult your surgeon if you have concerns.
Late Stage Bone Maturation: Months 2-6
- Characteristics: The grafted bone material integrates fully with your natural bone.
- Care: Regular check-ups with your dentist to monitor the graft’s success and to determine when it’s strong enough for the next steps, such as implant placement.
- Watch for: Persistent discomfort or signs that the graft isn’t integrating with your natural bone.
Understanding each dental bone graft healing stage can help you actively participate in your recovery. It will help you know when to return to normal activities, what symptoms to watch for, and when to consult your healthcare provider. This knowledge can contribute significantly to the success of the graft and any subsequent dental procedures, such as the placement of implants.
Tips for Accelerating Healing and Minimising Risks
Accelerating the healing process and minimising risks are important considerations after undergoing a dental bone graft. Here are some tips to ensure a smooth and successful recovery through the dental bone graft healing stages:
Medication Management
- Antibiotics: Take all prescribed antibiotics to prevent infection.
- Pain Relief: Use prescribed or over-the-counter pain medication as your surgeon advises to manage discomfort.
Optimal Oral Hygiene
- Soft Brushing: Use a soft-bristled toothbrush to avoid injuring the graft site.
- Antiseptic Rinse: Use prescribed antiseptic mouthwash to keep the surgical area clean.
Dietary Precautions
- Soft Foods: Stick to a soft-food diet initially to avoid putting pressure on the graft.
- Hydration: Drink plenty of fluids, but avoid using a straw, as the suction could disturb the graft.
Activity Restrictions
- Avoid Physical Strain: Limit strenuous activities for the first few days to a week after surgery.
- No Smoking: Smoking can inhibit healing and increase the risk of graft failure.
Regular Monitoring and Follow-Up
- Promptly Address Issues: Contact your healthcare provider at the first sign of abnormal symptoms like excessive pain or signs of infection.
- Scheduled Check-ups: Attend all follow-up appointments to ensure the graft is healing.
Additional Care
- Ice Packs: Use ice packs to minimise swelling during the first 48 hours.
- Elevate Head: Keep your head elevated, even during sleep, to minimise inflammation.
By actively participating in your recovery and following these guidelines, you can accelerate healing and minimise risks associated with dental bone grafts. Always consult your dental healthcare provider for personalised advice tailored to your needs and conditions.
References:
https://my.clevelandclinic.org/health/treatments/21727-dental-bone-graft
https://www.healthline.com/health/dental-bone-graft
https://www.cuh.nhs.uk/patient-information/bone-grafting-for-dental-implants/
https://www.mayoclinic.org/tests-procedures/dental-implant-surgery/about/pac-20384622